
Related Services
Our Office
Visit Us Online
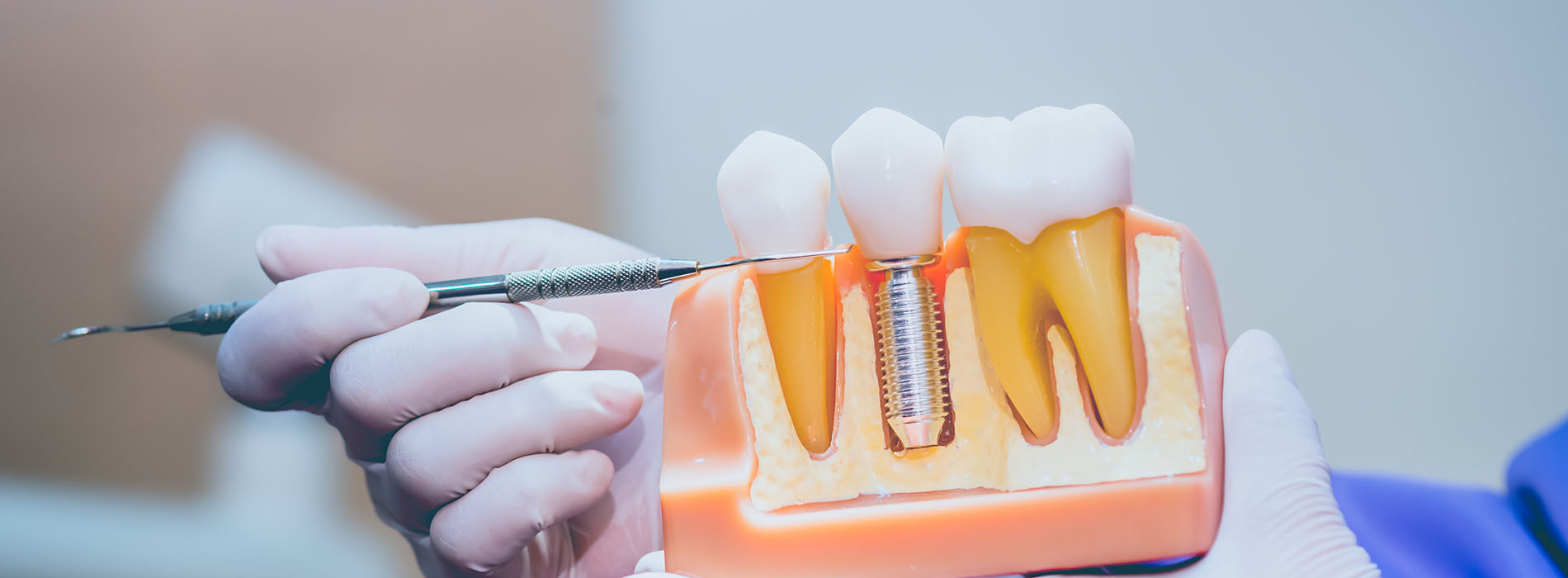
Implant restorations in east san jose play a critical role in completing the dental implant process by replacing the visible portion of a missing tooth while working in harmony with the implant beneath the gumline. At Suezaki Family Dentistry, this stage of treatment is focused on precision, comfort, and long-term oral stability. While the implant itself acts as an artificial tooth root, the restoration is what brings your smile back to full function and natural appearance.
For patients exploring implant dentistry in East San Jose, it is important to understand that restoration is not just cosmetic. It directly influences how you chew, speak, and maintain balance within your bite. A well-designed restoration helps distribute pressure evenly and supports the surrounding teeth and bone structure, creating a complete and functional smile that feels natural in everyday life.
Tooth loss affects far more than aesthetics. When a tooth is missing, the surrounding structures begin to shift, and the jawbone in that area may gradually weaken. Implant restorations address these challenges by restoring both structure and function in a way that closely replicates a natural tooth.
Replaces missing tooth structure so you can eat comfortably and evenly distribute bite pressure
Works with the implant post to help preserve bone density over time
Prevents drifting or shifting that can affect bite balance
Helps restore proper tongue placement and airflow during speaking
Reduces strain on remaining teeth and supports overall stability in the mouth
These benefits make implant restorations in east san jose a foundational part of modern restorative dentistry, especially for patients looking for a long-term solution rather than a temporary fix.
The restorative phase is highly customized because every patient’s bite, bone structure, and smile line are unique. At Suezaki Family Dentistry, each restoration is carefully designed to blend with surrounding teeth while ensuring proper function and comfort.
This process ensures that implant restorations in east san jose do not simply fill a gap but instead rebuild a natural-looking and fully functional tooth replacement.
| Type of Restoration | What It Replaces | How It Functions | Common Use Case |
|---|---|---|---|
| Single Crown | One missing tooth | Attaches to a single implant to mimic natural tooth function and aesthetics. | Isolated tooth loss where surrounding teeth are healthy. |
| Implant Bridge | Multiple missing teeth | Spans across two or more implants to restore a continuous section of teeth without needing natural anchors. | Replacing a row of adjacent missing teeth. |
| Implant Denture | Full arch (top or bottom) | Secures a removable or fixed prosthetic using 4 to 6 implants for maximum stability. | Extensive or total tooth loss where traditional dentures lack stability. |
Each type of restoration is designed to restore stability while maintaining a natural feel in the mouth, making dental implants in East San Jose a versatile solution for a wide range of patients.
Once the implant has fully integrated with the jawbone, the focus shifts to building the final tooth structure. This phase is generally comfortable and involves fewer invasive steps compared to implant placement.
During this stage, small refinements are often made to ensure the restoration feels natural when speaking and chewing. The goal is for the final result to function as if it has always been part of your smile.
Material selection plays an important role in durability, comfort, and appearance. The most commonly used materials are chosen for their ability to withstand daily function while maintaining a natural look.
Each material is selected based on location in the mouth, bite pressure, and cosmetic goals, ensuring that implant restorations in east san jose are both functional and visually seamless.
Caring for implant restorations is similar to maintaining natural teeth, but it requires consistent attention to the surrounding gum tissue. Healthy gums are essential for long-term implant stability.
With proper care, implant restorations can remain strong and functional for many years, supporting both oral health and daily comfort.
At Suezaki Family Dentistry, implant restorations are approached as the final and most personalized stage of implant treatment. Every restoration is designed with attention to detail so that it integrates naturally with your bite, facial structure, and overall smile.
By combining advanced planning, modern materials, and a patient-centered approach, dental implants in East San Jose are restored in a way that prioritizes both longevity and natural function. The result is a smile that feels stable, looks natural, and supports long-term oral health.
Implant restorations offer a reliable and predictable way to complete your dental implant journey. Whether replacing a single tooth or multiple teeth, the goal is always to restore balance, comfort, and confidence in everyday life.
If you are considering implant restorations in east san jose, Suezaki Family Dentistry is here to guide you through every stage with clarity and care.
Implant restorations are prosthetic teeth that attach to dental implants, replacing the visible portion of a missing tooth or teeth while the implant serves as an artificial root. The implant integrates with the jawbone through a process called osseointegration, creating a stable foundation for a crown, bridge or overdenture. Restorations are designed to recreate natural tooth form and function, including chewing, speech and the appearance of the smile.
Because implant restorations are anchored to implants rather than relying on adjacent teeth for support, they help preserve surrounding tooth structure and facial support. They also distribute chewing forces in a way that can protect remaining teeth and reduce bone loss at the site of the missing tooth. When planned and executed properly, implant restorations provide durable, lifelike results that blend with the rest of the dentition.
Candidacy for implant restorations begins with a comprehensive clinical exam that evaluates bone volume, gum health and overall medical conditions that affect healing. Many patients who have lost one or more teeth are candidates, provided there is sufficient bone to support an implant or that bone grafting can be performed to rebuild deficient sites. Your dentist will also review oral hygiene habits and any history of periodontal disease to determine the best path forward.
Age alone is not a limiting factor, but certain systemic conditions or medications can influence the timing and predictability of treatment, so open communication with your dental and medical providers is important. Smokers and patients with uncontrolled diabetes may require special consideration or adjunctive care to improve outcomes. A personalized evaluation helps identify whether single crowns, implant-supported bridges or implant-retained overdentures are the most appropriate option.
Implant restorations include single crowns that replace one tooth, implant-supported bridges that span multiple missing teeth, and implant-retained overdentures for patients missing most or all teeth. The restorative design is chosen based on how many teeth are missing, available implant sites and the patient’s functional and aesthetic goals. Each format distributes chewing forces differently and has distinct advantages in terms of stability and maintenance.
Restorations can also be categorized by how they connect to the implant: screw-retained or cement-retained designs are common and each has clinical trade-offs. Screw-retained prostheses are often easier to access for adjustments or repairs, while cement-retained options can offer specific esthetic or occlusal advantages depending on the case. Your restorative dentist will explain which configuration best suits your long-term needs.
Planning for implant restorations typically involves 3D imaging and digital or conventional impressions to precisely map bone anatomy, implant position and neighboring teeth. Treatment planning often occurs in collaboration between the surgical and restorative teams so that implant placement anticipates the final prosthetic design, emergence profile and gum support. This interdisciplinary approach reduces surprises and improves the predictability of the final outcome.
Digital workflows, including intraoral scanning and virtual implant planning, allow for more accurate communication with dental laboratories and the fabrication of custom abutments and provisional restorations. A well-executed plan includes timing for any preparatory procedures such as bone grafting or soft tissue management, and sets expectations for healing intervals and restoration sequencing. Clear communication about daily habits and long-term goals helps tailor the plan to each patient.
Implant restorations are made from a range of materials chosen for strength, esthetics and biocompatibility, including high-strength ceramics like zirconia and lithium disilicate and titanium components for internal strength. Ceramic materials offer lifelike translucency and color matching for front teeth, while zirconia and layered restorations can provide additional toughness in posterior areas where chewing forces are greater. Material selection balances the desire for a natural appearance with the need for long-term durability.
Other factors such as the thickness of the ceramic, the design of the restoration and the type of abutment influence how a restoration looks and performs. Metal-free options are often preferred in visible areas for better esthetics, while hybrid designs that incorporate metal or titanium can optimize mechanical performance where needed. Your clinician will recommend materials based on the location of the tooth, bite forces and your esthetic expectations.
Once the implant has successfully integrated with the bone and your clinician confirms stable healing, the restoration phase begins with precise impressions or digital scans of the implant and surrounding teeth. A custom abutment is fabricated to support the crown or bridge and to create an appropriate emergence profile for healthy gum tissue. Often a provisional restoration is placed first to refine shape, function and esthetics before the final prosthesis is made.
Fitting the permanent restoration involves verifying fit, occlusion and contact with adjacent teeth and making any necessary adjustments to ensure comfort and function. The restoration is then secured to the implant with a screw or cement, and final polishing and occlusal checks are completed. After placement, the team confirms that chewing function is restored and that the restoration integrates visually with the smile.
Daily oral hygiene is essential to protect implant restorations and the surrounding tissues; patients should brush gently with a soft-bristled brush and clean interdental spaces with floss or specially designed interdental brushes. Cleaning around the abutment and contact areas helps prevent plaque accumulation and inflammation of the soft tissues, which can compromise implant health over time. Avoid using metal instruments or abrasive pastes on ceramic surfaces to preserve the restoration finish.
Patients with a history of grinding or clenching should discuss protective measures such as a night guard to limit excessive forces on the restoration and implant components. Habits like chewing ice, opening packages with teeth or biting hard objects should be avoided to reduce the risk of chipping or mechanical failure. Consistent home care combined with regular dental monitoring is the best strategy for long-term success.
Regular professional maintenance includes periodic dental exams, professional cleanings and radiographic evaluations to monitor bone levels and the condition of the restoration. Dental hygienists use instruments and techniques that safely remove biofilm around implant components without damaging the prosthesis. These visits also allow your clinician to identify early signs of soft tissue inflammation, loose components or occlusal changes that may require intervention.
Maintenance intervals are individualized based on risk factors such as history of periodontal disease, smoking status and systemic health, but most patients benefit from at least biannual evaluations. During these appointments, the dentist will check screw torque on screw-retained restorations, evaluate cement margins for excess cement on cement-retained restorations and advise on any needed repairs or adjustments. Prompt attention to small issues helps prevent more significant complications.
While implant restorations have a high success rate, potential complications include biological issues like peri-implant mucositis and peri-implantitis, as well as mechanical problems such as screw loosening or prosthetic fracture. Peri-implant mucositis is inflammation of the soft tissue around the implant and can progress to bone loss if left untreated, whereas mechanical failures often result from excessive occlusal forces or improper restorative design. Early detection and management are key to addressing these problems conservatively.
Signs to watch for include redness, swelling, bleeding on probing, persistent discomfort or changes in how the restoration feels when biting. If any of these symptoms occur, patients should seek evaluation promptly so that noninvasive measures can be taken when possible. Good oral hygiene, regular professional care and appropriate protective measures reduce the likelihood of complications and support long-term success.
To begin, schedule a consultation so the clinical team can perform a comprehensive oral exam and necessary imaging to evaluate bone, gum health and overall suitability for implant restoration. During the consultation your dentist will discuss restorative options, the expected sequence of treatment and any preparatory procedures that may be needed to achieve a predictable result. This visit is an opportunity to review your goals, ask questions and establish a customized plan that aligns with your oral health needs.
If you choose to proceed, the team will coordinate surgical and restorative appointments and outline the timeline for healing and final restoration placement. The office in San Jose uses modern diagnostic tools and digital workflows to improve accuracy and esthetic outcomes, and the restorative phase is tailored to provide natural-looking, long-lasting results. Contact the office of Suezaki Family Dentistry to arrange an evaluation and learn which implant restoration approach is right for you.
